Patient-Reported Outcome Measures (PROMs)
PROMs calculate the health gains after surgical treatment from a patient perspective.
This can contribute to the analysis of revision rates, identifying patients with persistent pain or disability as well as measuring patient satisfaction after surgery. Therefore, many registries and hospitals have started to record PROMs data. There is a growing demand for feasible methods and instruments to collect comprehensive PROMs and to enable data comparison between the registries.
Patient reported outcome PROMs including pain and function data have been collected nationally by NHS Digital since 2009 for all patients receiving a primary hip or knee replacement. This information has not been included in the NJR Annual Reports yet, but shall be addressed in future annual reports.1
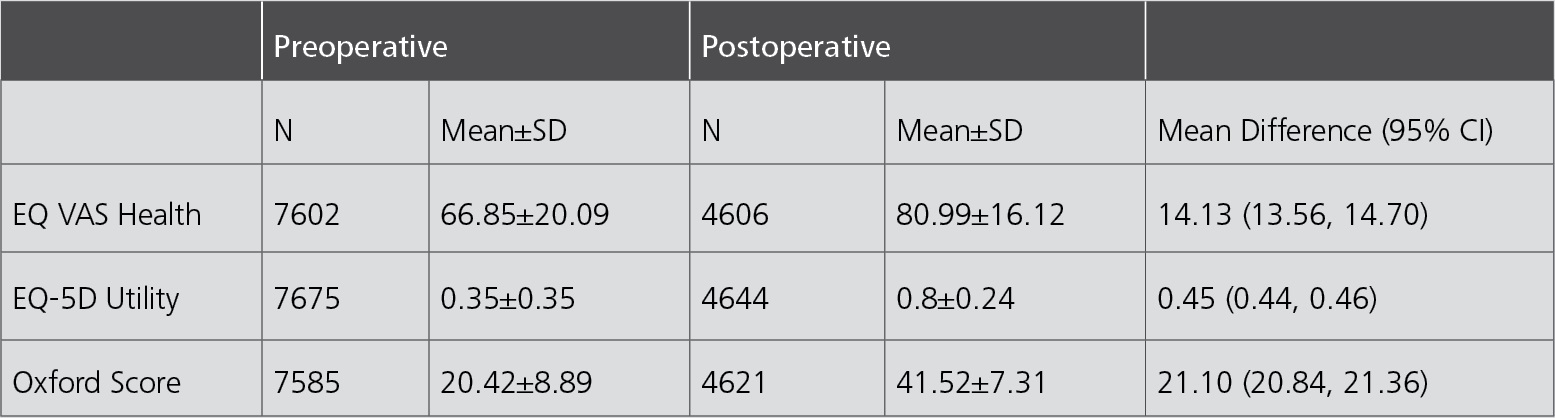
The Australian registry conducted a pilot program to determine the feasibility of collecting PROMs from patients undergoing hip, knee or shoulder arthroplasty in 2017 involving 44 hospitals. The national roll-out of PROMs data collection started in 2020. For THR patients, the validated PROMs reported in 2020 include the EQ-5D Utility Index. This summary score
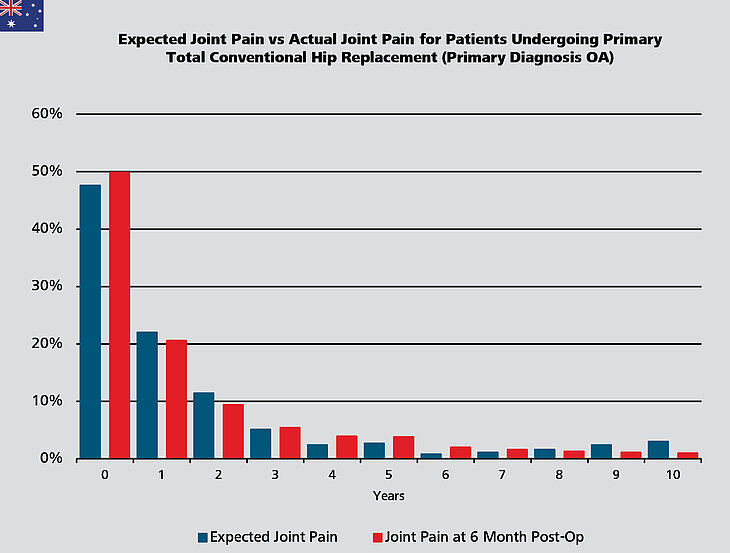
is generated from the five domains of the EQ-5D survey: usual activities, mobility, pain, depression/anxiety and quality of life. Its values span from 0 (‘a state as bad as being dead’) to 1 (‘full health’). Another included score, the EQ VAS Health, is a measure of patient-reported health ‘today’, ranging from 0 (‘worst health imaginable’) to 100 (‘best health imaginable’). The Oxford Score provides joint-specific values of pain and function, ranging from the worst possible 0 to a maximum of 48, complemented by preoperative expectations and patientperceived improvement at 6 months. For both surgeon-level and hospital-level of patients’ proportion who indicated that they were satisfied, the overall rate of satisfaction for THR was 87%, respectively.2
290 sites out of 1,152 (25.2%) have submitted PROMs until December 31, 2020, marking a 39% increase compared to the previous Annual Report. Based on the HOOS JR. score, 93% of the patients achieved a meaningful improvement after elective primary THR. The HOOS JR., PROMIS-10, and VR-12 scores are the main instruments used by the AJRR to record PROMs after hip replacement.4
The NZJR was one of the first joint registries to collect PROMs data. The validated Oxford Hip outcome questionnaires have been sent out on a random selection basis since July 2002 achieving an annual response rate of 20%. It was agreed that in the future, the questionnaires should be sent to all registered patients six months following surgery and after that at five-year intervals.
The NZJR uses the Oxford-12 questionnaire which includes 12 questions with score points ranging from 4 to 0. The maximum score of 48 indicates normal function, 0 stands for most severe disability. At six months after surgery, 84% of the participants have an excellent or good score. The average numbers are 42.37, 41.94, 41.37 and 40.75 at five, ten, fifteen and twenty years, respectively, after surgery.5
In Sweden, the PROM-routine for hip replacement started as a pilot project in one region in 2002. Until 2020, more units joined, then PROMs were registered for more than 50% of the primary surgeries. In 2017, EQ-5D-5L was used to get health-related quality of life. Since 2012, the SAR started “Supported Osteoarthritis Self-Management Program”, and in 2013 a question of smoking was added. At one, six, and ten years after the latest surgery, the same PROM-questionnaire with the addition of one question is sent to the patient.6
Latest registry data confirm former findings and existing trends. Hybrid fixation is gaining popularity. The same is true for dual mobility, especially in the treatment of fractured neck of femur. There is a modest comeback for hip resurfacing: While the use of the metal-on-metal version is restricted to patients meeting very strict selection criteria, the newly introduced ceramic-on-ceramic resurfacing could become a game changer.
Dual Mobility
AJRR, AOA NJRR, EPRD, NJR, and SAR are reporting the usage of dual mobility bearings, which have steadily increased over the years.1-4 In Australia, dual mobility prostheses show a lower rate of revision for dislocation than all other acetabular prostheses.2 The American registry reports that dual mobility constructs were mostly used in patients younger than 50 years, accounting for 9.4% of the cases.4 According to the NJR, the CoPoM dual mobility bearing shows lower revision rates than the MoPoM combination but without significant difference.1 According to the EPRD Annual report 2020 and 2021, the modular and dual mobility cup systems have increased their share from 0.4 % to 1.2 % in the period 2015-2020.17,18
Hip Resurfacing
Metal-on-metal resurfacing is still restricted to carefully selected patients. Women are mostly excluded from this procedure. Ceramic resurfacing procedures are recorded in the NJR and AOA NJRR. According to the NJR, currently performed CoC and MoP resurfacing procedures will be reported as a new category in future reports although the numbers are likely to remain too small for meaningful analysis for some years.
In the Australian registry, 177 CoC hip resurfacing procedures are documented, showing a cumulative revision rate of 0.6 (0.1, 4.2) at 1 year. This number is lower than that of MoM resurfacing at 1 year.2 The 2020 Annual Report states that ‘metal related pathology is the most common reason for revision after 7 years‘.12 Using ceramic instead of metal should therefore potentially minimize the major risks and contraindications for hip resurfacing. In New Zealand, the use of MoM-resurfacing has continuously increased from 70 procedures in 2016 to 122 procedures in 2020.5
Hybrid Fixation
According to the NJR, hybrid fixation has become the most popular choice for hip replacement for the first time.1 Hybrid fixation combined with CoP is the most frequently utilized construct in 2020 documented by the NJR. CoC bearings with hybrid fixation have a lower long-term revision rate than other combinations.1 The percentage of hybrid fixation documented in Australia has increased slightly from 34.8% in 2003 to 36.8% in 2020. For patients aged 75 years or older the revision rate is lower when either hybrid or cemented fixation is used, with the analysis restricted to modern prostheses.2
1. National Joint Registry. 18th Annual Report 2021 Surgical data to 31 December 2020. ISSN 2054-183X (Online) 2021: 1-376.
2. Australian Orthopaedic Association National Joint Replacement Registry (AOANJRR). Hip, Knee & Shoulder Arthroplasty: 2021 Annual Report, Adelaide; AOA, 2021: 1-432. [Accessed from: aoanjrr.sahmri.com/annual-reports-2021].
3. Endoprothesenregister Deutschland (EPRD). Jahresbericht 2021 Mit Sicherheit mehr Qualität. ISBN: 978-3-9817673- 9-1 2021: 1-193.
4. American Joint Replacement Registry (AJRR): 2021 Annual Report. Rosemont, IL: American Academy of Orthopaedic Surgeons (AAOS), 2021.
5. The New Zealand Joint Registry. Twenty-two year report January 1999 to December 2020. 2021: 1-196.
6. The Swedish Arthroplasty Register. Annual report 2021. ISSN 1654-5982. 2021: 1-224.
7. Australian Orthopaedic Association National Joint Replacement Registry. Annual Report. Adelaide: AOA; 2015.
8. Australian Orthopaedic Association National Joint Replacement Registry. Annual Report. Adelaide: AOA; 2016.
9. Australian Orthopaedic Association National Joint Replacement Registry (AOANJRR). Hip, Knee & Shoulder Arthroplasty: 2017 Annual Report. Adelaide: AOA, 2017.
10. Australian Orthopaedic Association National Joint Replacement Registry (AOANJRR). Hip, Knee & Shoulder Arthroplasty: 2018 Annual Report. Adelaide: AOA, 2018.
11. Australian Orthopaedic Association National Joint Replacement Registry (AOANJRR). Hip, Knee & Shoulder Arthroplasty: 2019 Annual Report. Adelaide: AOA, 2019.
12. Australian Orthopaedic Association National Joint Replacement Registry (AOANJRR). Hip, Knee & Shoulder Arthroplasty: 2020 Annual Report, Adelaide; AOA, 2020: 1-474. [Accessed from: aoanjrr.sahmri.com/annual-reports-2020].
13. Endoprothesenregister Deutschland (EPRD). Statusbericht 2014 Mit Sicherheit mehr Qualität. 2015: 1-60.
14. Endoprothesenregister Deutschland (EPRD). Jahresbericht 2015 Mit Sicherheit mehr Qualität. ISBN: 978-3-9817673-1-5. 2016: 1-65.
15. Endoprothesenregister Deutschland (EPRD). Jahresbericht 2016 Mit Sicherheit mehr Qualität. 2017: 1-64.
16. Endoprothesenregister Deutschland (EPRD). Jahresbericht 2017 Mit Sicherheit mehr Qualität. ISBN: 978-3-9817673-3-9. 2018: 1-80.
17. German Arthroplasty Registry (EPRD). 2019 Annual Report. 2020: 1-125. doi:10.36186/reporteprd01202.
18. Endoprothesenregister Deutschland (EPRD). Jahresbericht 2020 Mit Sicherheit mehr Qualität. 2020: 1-128.doi:10.36186/reporteprd022020.
19. Davis ET, Pagkalos J, Kopjar B. Effect of bearing surface on survival of cementless and hybrid total hip arthroplasty: study of data in the National Joint Registry for England, Wales, Northern Ireland and the Isle of Man. JB JS Open Access. 2020;5(2):e0075. doi:10.2106/JBJS.OA.19.00075.
20. Davis ET, Pagkalos J, Kopjar B. A higher degree of polyethylene irradiation is associated with a reduced risk of revision for aseptic loosening in total hip arthroplasties using cemented acetabular components: an analysis of 290,770 cases from the National Joint Registry of England, Wales, Northern Island and the Isle of Man. Bone Joint Res. 2020;9(9):563-571. doi:10.1302/2046-3758.99.BJR-2020-0135.R1.
21. Paxton EW, Cafri G, Nemes S, et al. An international comparison of THA patients, implants, techniques, and survivorship in Sweden, Australia, and the United States. Acta Orthop. 2019;90(2):148-152. doi:10.1080/17453674.2019.1574395.